
3 reasons to take a patient-centric approach to weight health management
A patient-centered holistic approach for weight loss management strategies can help create savings for plans and members. Here are three things to consider.
In the ever-evolving healthcare landscape, employers, PBMs, and even members find themselves at a crossroads when it comes to weight loss management. Obesity in the U.S. should be treated as a chronic condition – and an expensive one. Due to associated comorbidities, obesity in the U.S. is calculated to be at least a $1.7 trillion disease, including $1.24 trillion in lost productivity and $480.7 billion in direct health care costs.
The path forward? A patient-first mindset paired with tech-savvy solutions. Here are three ways a shift in perspective on weight loss management can pave the way for better outcomes.
Break free from rebate-driven formularies
Issue: Legacy organizations who offer pharmacy benefits often prioritize rebates. Their formularies may favor a single highly rebated drug, leaving patients with limited options. While this approach may boost short-term financial gains, it can fail both plans and patients. Why? Because it disregards the patient’s financial constraints and health needs.
Solution: Embrace a holistic view. Consider a plan that focuses on lowering net cost but also weighs patient affordability and clinical effectiveness. By diversifying formularies, we can empower patients with choices that align with their unique circumstances.

Empower patients from the point of prescribing on their weight health journey
Issue: Picture this: A patient receives a prescription, heads to the pharmacy, and faces sticker shock at the checkout counter. Why? Because the current prescription experience keeps patients in the dark about medication prices until it’s time to pay. It’s a disservice to those seeking care.
Solution: Transparency is key. Imagine a world where patients know the cost of their medication the moment it’s being prescribed — before they reach the pharmacy. Technology allows us to provide real-time pricing information, empowering patients to make informed decisions and engage in better conversations with their provider at the point of care.

Unravel complexity created by discount cards
Issue: Discount card programs abound, promising savings, which can be particularly attractive for expensive weight loss drugs. But navigating this complex landscape can leave patients confused. Patients shouldn’t have to hunt for information and be left guessing about costs.
Solution: Streamline the experience. Imagine a seamless process where patients compare cash prices versus insurance-covered costs— all from their smartphones. By demystifying pricing, we empower patients to see all their options and pick the way they want to pay.

The Prescryptive way:
Include the patient upfront in the process
At Prescryptive, we believe the patient needs to be an active participant in their healthcare experience and be fully informed and engaged to have the best outcomes.
So, even if you have a great weight loss management solution between your medical and pharmacy benefits, and you’re engaging a physician, you are still missing the most important part of the equation — and that is the patient. The patient should be informed on costs at the point of care.
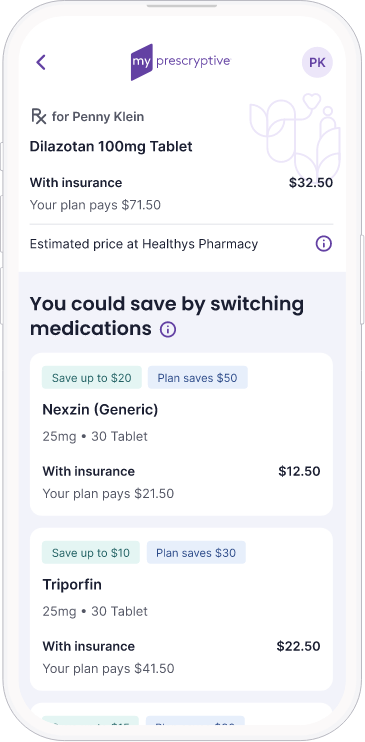
What’s more, they should know how their plan is supporting them with costs. Because patients might think differently about the cost of a certain weight management drug if they know that their plan is paying $1,000 per prescription (just for example). This information might place some accountability on the patient — and it might give them deeper appreciation for the plan and benefits provided, too.
And, if a medication is prescribed without the patient being part of the process, the plan could wind up paying for a higher priced medication when the patient could have started on a lower cost option to monitor their results and reactions first.
Let’s connect to rewrite the script, together
Let’s put patients at the center, armed with information and empowered to choose wisely. By bridging the gap between legacy practices and patient-centric innovation, we can transform healthcare—one prescription at a time.
Rae McMahan is the SVP, Payer Solutions, at Prescryptive Health.
