Rewriting the script for
Who we serve
We keep your patients engaged in their health journeys, increasing adherence with our easy-to-integrate platform.
Better profitability for your pharmacy and better prices for your patients starts with our AI-optimized pricing tool.
More than a PBM – emPBM helps empower employers, employees, and members.
Gain insights about patients to align and inform with your brand name strategy.
No more pharmacy surprises. Know the price of your prescriptions before you even leave the doctor’s office.
We believe in the impact of patient engagement
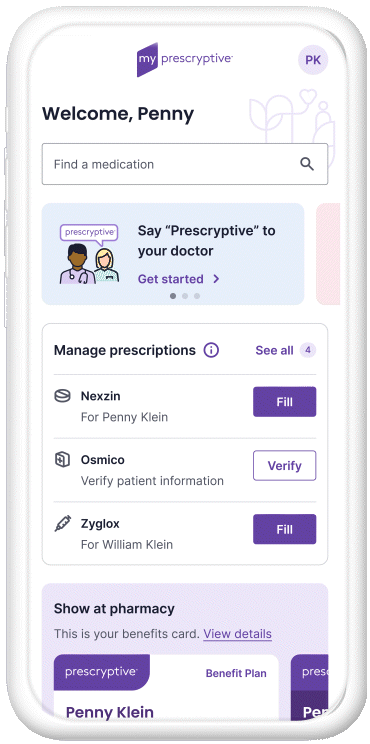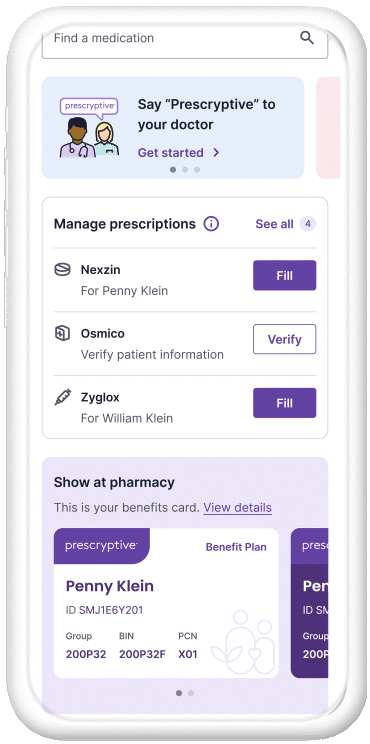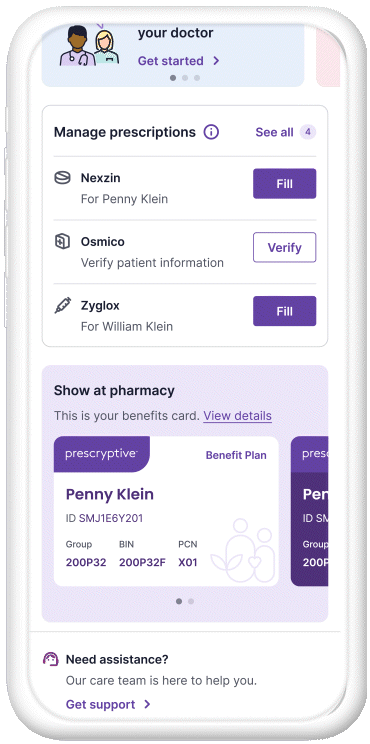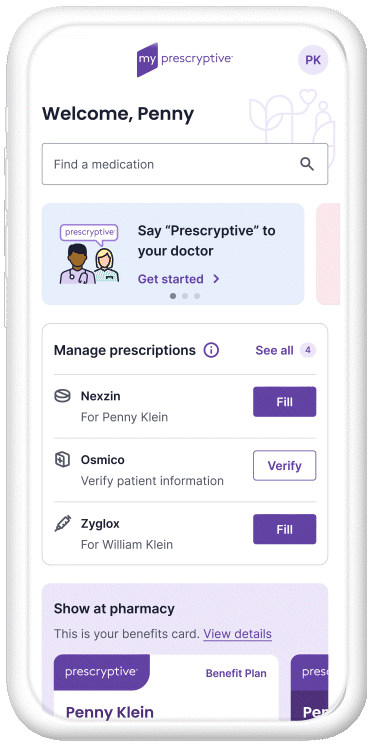
The myPrescryptive healthcare platform uses advanced technology to give patients power over their prescriptions, and their health.
Our platform
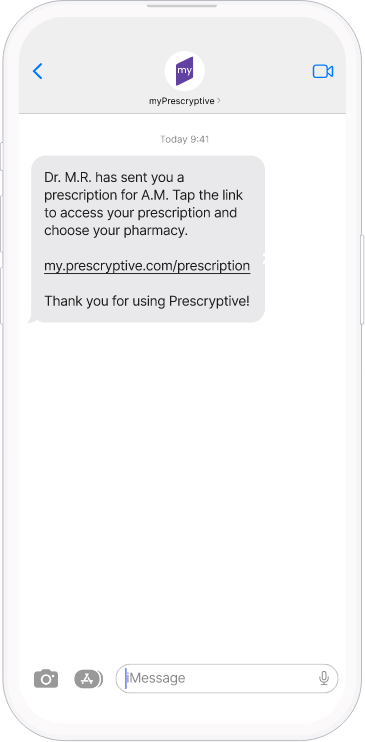
Empowerment at the point of care
With myPrescryptive, patients receive real-time text alerts that help them make better, more informed decisions.
- Prescriptions are delivered right to the patient’s phone
- Intelligent alerts help patients find the better-priced alternatives
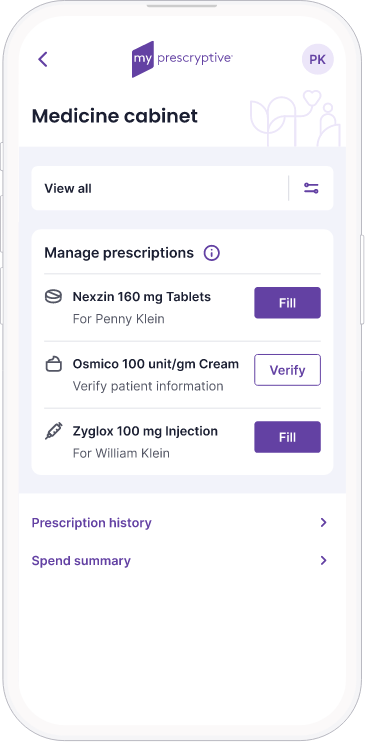
Managing prescriptions for better outcomes
Patients track and manage their prescriptions on a convenient, secure platform — no app to download.
- Digital medicine cabinets for individuals and families
- Build a prescription history and keep track of it
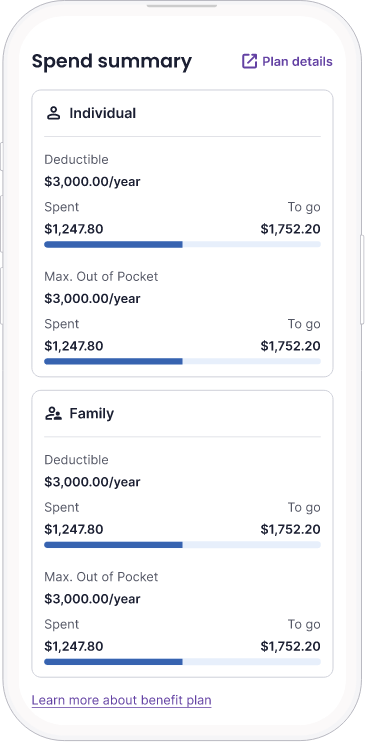
Track healthcare spending
Our spend summary tool helps patients demystify their deductibles and keep track of their plan details.
- Transparency helps patients take control of their prescriptions
- Informed decision making helps patients adhere to medications to improve health outcomes
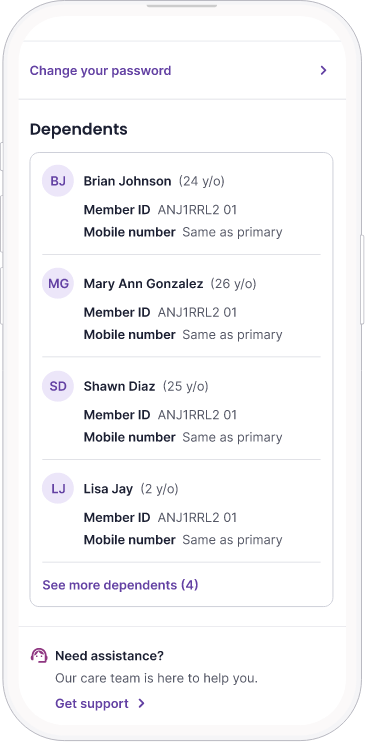
Manage prescriptions for dependents
Because care extends to loved ones, too.
- Easily manage prescription needs for the family all in one place – the phone
- Peace of mind for caregivers who need to transfer, fill, and shop for prescriptions securely
See what Prescryptive can do for you
Learn more about how we serve every step of the prescription process
“Before Prescryptive, we were fielding issues with our pharmacy benefit almost weekly.”



News & Insights
6 signs it’s time to replace your PBM & what to look for in a new solution
Employers may be hearing rumblings that it’s time to move on from the legacy PBMs in light of…
What is a digital prescription?
The days of paper prescriptions — when a patient got a piece of paper to carry from the…
REPORT: How AI is powering the pharmacy of the future
The data is in, and Prescryptive AI Pricing is driving profitability for America’s community pharmacies facing major headwinds,…
PODCAST: Pharmacy Technicians Solving Prescription Price Concerns
Prescryptive is proud to work with Kerrville Drug Co. in Texas, whose Pharmacy Manager and Certified Pharmacy Technician,…